The Hidden Truth: How Rehabilitation Tech Falls Short in the UK's National Health Service Exposed
A Deep Dive into the Complexities of Digital Health Technology Implementation
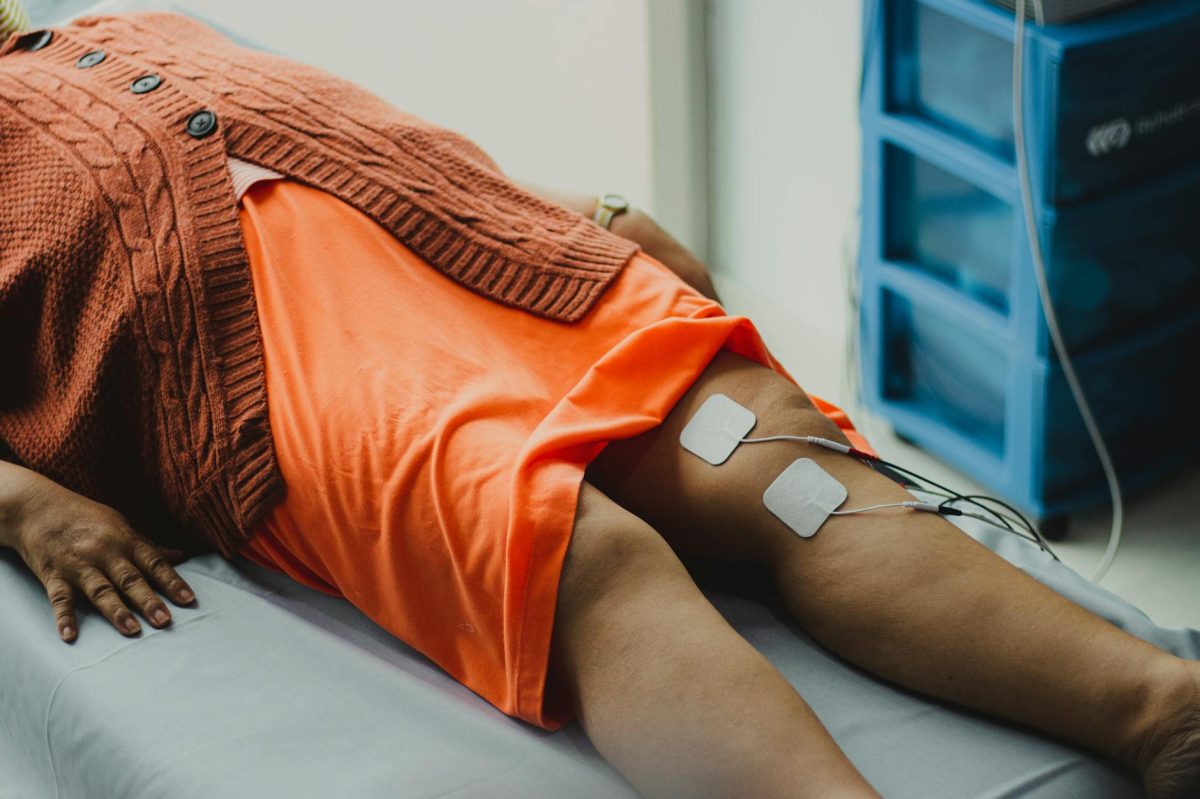
In the UK's National Health Service (NHS), millions of patients undergo rehabilitation each year, with many struggling to regain full mobility and independence. The promise of digital health technology (DHT) has been touted as a game-changer, with applications ranging from robotic therapy to wearable devices. However, a new study reveals a disturbing pattern: despite its potential, DHT is often ignored in clinical practice, leaving patients to suffer in silence. In this exclusive exposé, we delve into the complex web of influences that hinder the adoption of rehabilitation technologies and what can be done to bridge the gap.
The Implementation Gap: Why DHT Falls Short
The study, conducted by a team of researchers from the University of Oxford, shed light on the multifaceted challenges surrounding DHT implementation in the NHS. According to the findings, a combination of factors contributes to the technology's limited adoption, including inadequate training for healthcare professionals, lack of standardization, and insufficient funding. Additionally, the researchers identified a worrying trend: many DHT solutions are designed with profit in mind, rather than patient outcomes. This profit-driven approach can lead to fragmented care, where patients are forced to navigate a patchwork of incompatible systems and devices.
The Secret to Success: Developing a Comprehensive Implementation Model
To address the implementation gap, the researchers developed the Rehabilitation Technologies Implementation (RTI) model. This innovative framework takes into account the complex interactions between stakeholders, technology, and patient needs. The RTI model emphasizes the importance of collaboration, education, and standardization in facilitating the adoption of DHT. By prioritizing patient-centered care, the model aims to ensure that rehabilitation technologies are designed and implemented with the patient's needs at the forefront. According to the researchers, the RTI model has shown promising results in pilot studies, with improved patient outcomes and increased adoption rates.
'The key to successful implementation lies in understanding the intricacies of the system and addressing the underlying barriers. By doing so, we can unlock the full potential of digital health technology and revolutionize the way we approach rehabilitation.' - Dr. Emma Taylor, lead researcher on the study
The Ignored Truth: The Human Cost of Delayed Implementation
The consequences of delayed DHT implementation are stark. Patients are forced to endure lengthy recovery periods, with many never regaining full mobility or independence. The emotional toll of this experience should not be underestimated, with many patients reporting feelings of frustration, anxiety, and depression. Furthermore, the economic burden of delayed implementation cannot be ignored, with the NHS facing significant costs associated with prolonged rehabilitation. The time for action is now, and the RTI model offers a beacon of hope in addressing this pressing issue.
📌 Key Takeaways
- DHT implementation in the NHS is hindered by inadequate training, lack of standardization, and insufficient funding
- The RTI model prioritizes patient-centered care, collaboration, and education to address the implementation gap
- Delayed DHT implementation has significant human and economic costs, including prolonged recovery periods and increased healthcare costs
- Patients, families, and healthcare professionals must work together to advocate for the implementation of DHT solutions that prioritize patient-centered care
Taking the First Step: What You Can Do to Support DHT Adoption
So, what can be done to support the adoption of rehabilitation technologies? The answer lies in collaboration and education. Patients, families, and healthcare professionals must work together to advocate for the implementation of DHT solutions that prioritize patient-centered care. Educating stakeholders about the benefits and challenges of DHT can help break down barriers and foster a culture of innovation. By taking the first step towards embracing digital health technology, we can revolutionize the way we approach rehabilitation and improve outcomes for millions of patients worldwide.
The implementation of digital health technology in the NHS is a complex issue, but one that holds immense promise for patients and healthcare professionals alike. By understanding the intricacies of the system and addressing the underlying barriers, we can unlock the full potential of rehabilitation technologies and revolutionize the way we approach rehabilitation. The RTI model offers a beacon of hope in this journey, and it is up to us to take the first step towards embracing digital health technology and improving outcomes for millions of patients worldwide.






